
We Improve Your Quality of Life
Rheumatoid arthritis is an autoimmune disease that causes chronic inflammation of the joints. Rheumatoid arthritis can also cause inflammation of the tissue around the joints, as well as other organs in the body.
Autoimmune diseases are illnesses that occur when the body tissues are mistakenly attacked by its own immune system.
While rheumatoid arthritis is a chronic illness, meaning it can last for years, patients may experience long periods without symptoms.
Causes



- The cause of rheumatoid arthritis is unknown.
- Even though infectious agents such as viruses, bacteria, and fungi have long been suspected, none has been proven as the cause.
- Some scientists believe that the tendency to develop rheumatoid arthritis may be genetically inherited.
- It is suspected that certain infections or factors in the environment might trigger the immune system to attack the body’s own tissues, resulting in inflammation in various organs of the body such as the lungs or eyes.
- Regardless of the exact trigger, the result is an immune system that is geared up to promote inflammation in the joints and occasionally other tissues of the body.
- Immune cells, called lymphocytes, are activated and chemical messengers (cytokines, such as tumor necrosis factor/TNF and interleukin-1/IL-1) are expressed in the inflamed areas.
- Environmental factors also seem to play some role in causing rheumatoid arthritis.
- Recently, scientists have reported that smoking tobacco increases the risk of developing rheumatoid arthritis.
Symptoms
- The symptoms of rheumatoid arthritis come and go, depending on the degree of tissue inflammation.
- When body tissues are inflamed, the disease is active. When tissue inflammation subsides, the disease is inactive (in remission). Remissions can occur spontaneously or with treatment, and can last weeks, months, or years.
- During remissions, symptoms of the disease disappear, and patients generally feel well.
- When the disease becomes active again (relapse), symptoms return. The return of disease activity and symptoms is called a flare.
- The course of rheumatoid arthritis varies from patient to patient, and periods of flares and remissions are typical.
- When the disease is active, symptoms can include fatigue, lack of appetite, low grade fever, muscle and joint aches, and stiffness.
- Muscle and joint stiffness are usually most notable in the morning and after periods of inactivity.
- Arthritis is common during disease flares. Also during flares, joints frequently become red, swollen, painful, and tender. This occurs because the lining tissue of the joint (synovium) becomes inflamed, resulting in the production of excessive joint fluid (synovial fluid). The synovium also thickens with inflammation (synovitis).
- In rheumatoid arthritis, multiple joints are usually inflamed in a symmetrical pattern (both sides of the body affected).
- The small joints of both the hands and wrists are often involved. Simple tasks of daily living, such as turning door knobs and opening jars can become difficult during flares.
- The small joints of the feet are also commonly involved.
- Occasionally, only one joint is inflamed. When only one joint is involved, the arthritis can mimic the joint inflammation caused by other forms of arthritis, such as gout or joint infection.
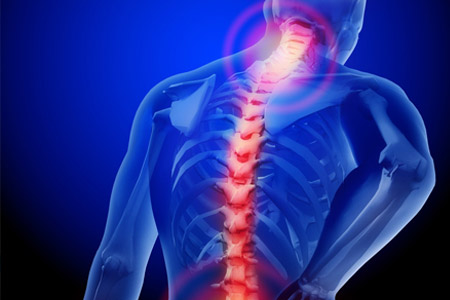
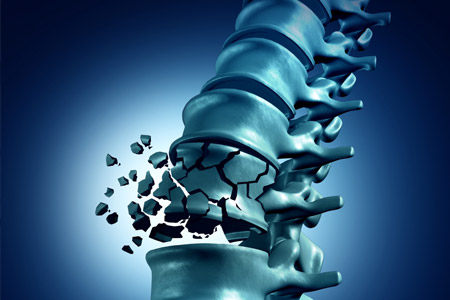
- Chronic inflammation can cause damage to body tissues, cartilage and bone. This leads to a loss of cartilage and erosion and weakness of the bones as well as the muscles, resulting in joint deformity, destruction, and loss of function.
- Rarely, rheumatoid arthritis can even affect the joint that is responsible for the tightening our vocal cords to change the tone of our voice, the cricoarytenoid joint. When this joint is inflamed, it can cause hoarseness of voice.


Diagnosis
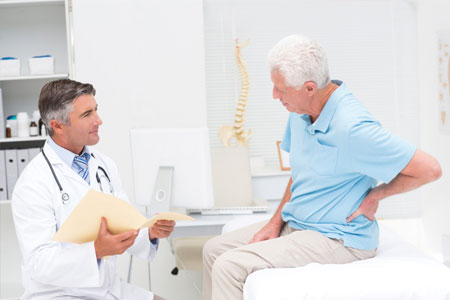
- History of symptoms
- Examination of the joints for inflammation and deformity
- Blood and x-ray tests
- The diagnosis is also based on the pattern of symptoms, the distribution of the inflamed joints.
- Bone scanning, a radioactive test procedure, can demonstrate the inflamed joints.
- Arthrocentesis can also be helpful in relieving joint swelling and pain.
Physioline management
At Physioline, all the members of the rehabilitation team work together so as to provide proper care and the therapy in order to:
- Pain relief
- Reduce swelling
- Strengthening of muscle
- Prescription of orthoses
Combination Therapy Is Only Answer for Rheumatoid Arthritis.

Why You must come to Physioline?
- Achieve Breakthrough Results.
- Fastest recovery time in India.
- Combination Therapy Usage for the first time in India.
- 17 years of Experience in Combating Pain.
- World-class Technological Advances under one roof.
Highlights of Our Treatment
- Innovative Programs to prevent Surgery.
- Unique treatment Approach for the first time in India.
- Continuous Up gradation of Professional skills and techniques.
- Patients could avoid surgical intervention in the past.
- Spinal Restoration implemented for medical tourism patients for the first time in India.
- Highest Success Percentages achieved in India.
Innovation with Expertise

Unmatched treatment Protocols for first time in India

Most Advanced Advances in India Technological

We aim to achieve highest level of patients satisfaction.

Videos Testimonials
Success Stories
I have taken specialized treatment of both my knees. At the end of my sessions I do feel appreciable change in the condition of my knees. I feel lightness in walking and lesser pain. I look forward to lead normal life after sometime with the treatment at Physioline. Thanks to Dr Sanjay Bakhshi and his team.Mrs Shashi Vohra Bilateral Osteoarthritis--- Both Knees
My name is Rekha Rawal and I am 56 year Old Lady. From last several months I had severe pain in my both Knees and also my Back was paining severely. I took treatment from various Doctors, but of no relief. After my son contacted to Dr. Sanjay Bakhshi from Physioline, he suggested me treatment for 30 days, & I started my treatment from Physioline. After 7 days of treatment I started feeling better, my pain had reduced and I started walking. Since before this treatment my walking had stopped as there was immense pain so with treatment the results were coming and the improvement was felt. Now after complete treatment, I have started walking and feeling better with new Life in my knees. I have received excellent results and treatment from Physioline.Mrs Rekha Raval Bilateral Osteoarthritis---Both Knees
I had begun to feel as if I am 70 at the age of 45 only. I would envy elderly people walking without any pain. Nothing seemed to help. My family was really disturbed on seeing my condition. I was diagnosed to be having early Osteo arthritis and the doctors advised to get the Physiotherapy done, but there was a long waiting period for treatment in U.k. I did not have the patience to bear so much pain so we decided to move to India for the Physical rehabilitation and we got the reference of Dr Sanjay Bakhshi, Physioline from one of our relative who had taken the treatment there. Thanks to Dr Bakhshi and his team who gave me complete pain relief and good recovery.Now I think that I can live without surgery by continuing to do all the prescribed exercises.Jayshree Chaudasama , UK Osteoarthritis, Knee---Physical Rehabilitation
