
Knee Osteoarthritis
Osteoarthritis is a type of arthritis that is caused by the breakdown and eventual loss of the cartilage of one or more joints. Cartilage is a protein substance that serves as a “cushion” between the bones of the joints. Osteoarthritis is also known as degenerative arthritis.
Osteoarthritis commonly affects the hands, feet, spine, and large weight-bearing joints, such as the hips and knees. Most cases of osteoarthritis have no known cause and are referred to as primary osteoarthritis. When the cause of the osteoarthritis is known, the condition is referred to as secondary osteoarthritis
Causes
- With aging, the water content of the cartilage increases and the protein makeup of cartilage degenerates. Repetitive use of the joints over the years irritates and inflames the cartilage, causing joint pain and swelling. Eventually, cartilage begins to degenerate by flaking or forming tiny crevasses. In advanced cases, there is a total loss of the cartilage cushion between the bones of the joints. Loss of cartilage cushion causes friction between the bones, leading to pain and limitation of joint mobility.
- Inflammation of the cartilage can also stimulate new bone outgrowths (spurs) to form around the joints.
- Osteoarthritis occasionally can be found in multiple members of the same family, implying an heredity (genetic) basis for this condition.
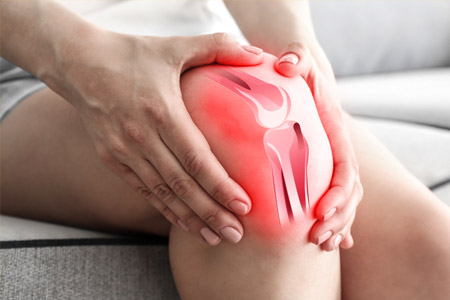
ON EXAMINATION
Swelling :
Due to synovial thickening/ effusion, muscle wasting, prominence of articular margins due to Osteophytes.
- Movements:painful & restricted.
- Crepitus: on joint movement .In later stages , loose bodies develop in the joint whicw may cause recurrent joint effusion, pain ,swelling & locking of the joint.


SYMPTOMS
The most common symptom of osteoarthritis is pain in the affected joint(s) after repetitive use. Joint pain is usually worse later in the day.
- There can be swelling, warmth, and creaking of the affected joints.
- Pain and stiffness of the joints can also occur after long periods of inactivity,
- Symptoms of osteoarthritis vary greatly from patient to patient. Some patients can be debilitated by their symptoms. On the other hand, others may have remarkably few symptoms in spite of dramatic degeneration of the joints apparent on x-rays.
- Osteoarthritis of the knees is often associated with obesity or a history of repeated injury and/or joint surgery. Progressive cartilage degeneration of the knee joints can lead to deformity and outward curvature of the knees referred to as “bow legged.”
- Patients with osteoarthritis of the weight bearing joints (like the knees) can develop a limp. The limping can worsen as more cartilage degenerates. In some patients, the pain, limping, and joint dysfunction may not respond to medications or other conservative measures.



Combination Therapy is the ONLY Answer for Knee Restoration to Prevent Surgery.
Surgical process has its own complications and patient realizes the same much after the surgery so first advice is to prevent the original knee with knee restoration program.

Why You must come to Physioline?
- Achieve Breakthrough Results to avoid Surgery
- Fastest recovery time in India.
- Combination Therapy Usage for the first time in India.
- 17 years of Experience in Combating Pain.
- World-class Technological Advances under one roof.
Highlights of Our Treatment
- Innovative Programs for faster recovery.
- Unique treatment Approach for the first time in India.
- Continuous Up gradation of Professional skills and techniques.
- Patients could avoid surgical intervention in the past.
- Knee Restoration implemented for medical tourism patients for the first time in India.
- Highest Success Percentages achieved in India.
Innovation with Expertise

Unmatched treatment Protocols for first time in India

Most Advanced Technological Advances in India

We can prevent Surgery with Timely treatment.

Videos Testimonials
Success Stories
My condition was so severe that my legs were not able to hold my body up, yet within couple of treatment session at Physioline I was mobile again. Now I walk with more confidence and my pain is completely vanished. Convenient and comfortable journey with Physioline.Dr.Sanjay Bakhshi was very supportive and talented. Really I am relieved from the problem. Equipments are highly updates. God bless the whole team of Physioline.Mrs.Shamsinisa Shaikh Knee pain
I have taken specialized treatment of both my knees. At the end of my sessions I do feel appreciable change in the condition of my knees. I feel lightness in walking and lesser pain. I look forward to lead normal life after sometime with the treatment at Physioline. Thanks to Dr Sanjay Bakhshi and his team.Mrs Shashi Vohra Bilateral Osteoarthritis--- Both Knees
My name is Rekha Rawal and I am 56 year Old Lady. From last several months I had severe pain in my both Knees and also my Back was paining severely. I took treatment from various Doctors, but of no relief. After my son contacted to Dr. Sanjay Bakhshi from Physioline, he suggested me treatment for 30 days, & I started my treatment from Physioline. After 7 days of treatment I started feeling better, my pain had reduced and I started walking. Since before this treatment my walking had stopped as there was immense pain so with treatment the results were coming and the improvement was felt. Now after complete treatment, I have started walking and feeling better with new Life in my knees. I have received excellent results and treatment from Physioline.Mrs Rekha Raval Bilateral Osteoarthritis---Both Knees
