
Introduction:
The muscular dystrophies (MD) are a group of X-linked genetic disorder characterized by progressive weakness and degeneration of the skeletal muscles that control movement.
Some forms of MD are seen in infancy or childhood, while others may not appear until middle age or later.
The disorders differ in terms of the distribution and extent of muscle weakness (some forms of MD also affect cardiac muscle), age of onset, rate of progression, and pattern of inheritance.
The genes for Duchenne’s and Becker’s MD are X-linked recessives – that is, they generally affect only boys but are carried and passed on by women.

Duchenne's muscular dystrophy (MD)

Most common and severe type is Duchenne’s muscular dystrophy (MD), in which a genetic defect leads to the formation of an abnormal type of muscle protein called dystrophin. Dystrophin is a protein involved in maintaining the integrity of muscle .This primarily affects boys. Onset is between 3 and 5 years and the disorder progresses rapidly. Most boys are unable to walk by age 12, and later need a respirator to breathe. Girls in these families have a 50 percent chance of inheriting and passing the defective gene to their children.
Types of Dystrophies
- Becker muscular dystrophy (BMD)
- Emery-Dreifuss muscular dystrophy
- Facioscapulohumeral muscular dystrophy
- Limb-Girdle muscular dystrophy
- Myotonic muscular dystrophy
- Oculopharyngeal muscular dystrophy
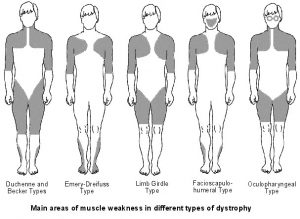
Symptoms of Muscular Dystrophy
Parents often first begin to suspect that a child has muscular dystrophy when they are about 3 to 6 years old and they notice that their child is frequently falling down has difficulty getting up when he is sitting or lying down has difficulty climbing stair climb a delay in walking on his enlarged calf muscles (pseudo hypertrophy)is walking on his toes in a kind of ‘waddle’walks with his shoulders pushed back (lordosis)gets easily tired during or after routine physical activities.
Obesity


Clinical Features of Muscular Dystrophy
Symptoms begin to show in pre-school boys.
First, the legs are affected, causing walking difficulties and balance problems.
As the disease progresses, the calves begin to swell with fibrous tissue rather than with muscle, and feel firm and rubbery. For this reason, DMD is also known as pseudohypertrophic muscular dystrophy.
By age five or six, the child will have contractures (permanent muscle tightening), mostly in the calf muscles.
This tightening pulls the foot down and back, so the child must walk on tip-toes.
By age nine or ten, it becomes difficult to climb stairs or stand without help.
By age 12, most boys use a wheelchair.
Scoliosis (a side-to-side spine curvature) and (a front-to-back curvature) often appear at this time.
DMD also causes diaphragm weakness, so it is difficult to breathe and cough. This affects the child’s energy level and increases lung infections.
DIAGNOSIS:
list of diagnostic tests
-Muscle biopsy
-Electromyography
TREATMENT AT PHYSIOLINE:
At Physioline, Muscular Dystrophy is treated with “COMBINATION THERAPY“
Combination Therapy ensures that the finest of rehabilitation is implemented which will improve the life span of the patient and also improve the quality of life to a maximum extent.
There are things that teens with MD can do to help their muscles. Certain exercises and physical therapy can help:To avoid contractures.


A stiffening of the muscles near the joints that can make it harder to move and can lock the joints in painful positions.
Often, teens are fitted with special braces to ensure flexible joints and tendons (the strong, rubber band-like tissues that attach muscles to bones).
Because we rely on certain muscles to breathe, some teens with MD need respiratory aids, such as a ventilator, to help them breathe.
Teens with MD also might need to be treated for problems like scoliosis, which can be caused by weakened muscles or muscles that are contracting or pulling too tightly.
With the help of a ventilator, patients with DMD often live into their twenties and beyond.
About one third of DMD patients have some learning disabilities that require individualized educational plans.
SELF-CARE TIPS OF PHYSIOLINE
There is currently no way to prevent muscular dystrophy if you have inherited the genes responsible for these disorders. However, accurate genetic tests are now available for the muscular dystrophies for which the mutated gene has been identified. These can be useful for family planning purposes for those with a family history of this disease. If you have been diagnosed with a form of muscular dystrophy, good nutrition is an important part of your general health.

Combination Therapy is the ONLY Answer for Muscular Dystrophy


Video Testimonial
Success Stories
My 6 months old daughter was diagnosed for delayed milestones. She was unable to hold her head, turn to one side. I was very much worried for my little girl. This was leading to depression. My daughter’s Paediatrician told me that Physiotherapy treatment would help her. As said by the Dr. I started my hunt for a Paediatric Physiotherapy Centre. I came to know about Physioline on the net. I consulted DR.SANJAY BAKHSHI – the chief consultant at physioline. He assured me that my baby has good scope of recovery with the kind of treatment they provide. As the days passed my baby started holding the head and was able to turn on one side, I could see a noticeable progress in her. All thanks to DR SANJAY BAKHSHI and his dedicated team at Physioline.MRS .SAJIDA KHAN Bhopal India Delayed milestones.
My 2 yr old son was diagnosed with Cerebral Palsy. After we got the diagnosis my husband and I felt like we have been punched in the stomach. My son’s Paediatrician told us my son needs vigorous Physiotherapy on daily basis. I came to know about Physioline through one of my friend. Dr. SANJAY BAKHSHI at Physioline started the ‘Combination Therapy’ for my son. Very soon after the treatment, my son’s condition significantly improved. He has improve arm and hand mobility. He comes up with new words. Dr. SANJAY BAKHSHI continues to keep detailed records to eventually provide evidence of my son’s new development. I would advise other parents in a similar situation to do the same.ISHITA PATEL Gujarat India. Cerebral Palsy
My 11 yr old son has been diagnosed for dyslexia. He had difficulty to listen, absorb and Concentrate on the task at hand. But after taking the treatment sessions at Physioline he has the ability to keep himself focused and to resist distractions. Through this program, my son is now a thriving, self-confident, self assured student that now knows he has the ability to achieve whatever he desires.MRS. SANGEETA Mumbai Dyslexia
